$99 New Patient Special - Includes Exam, X-Ray and Basic Cleaning
What Is a Root Cavity? Causes, Signs, and Prevention Tips
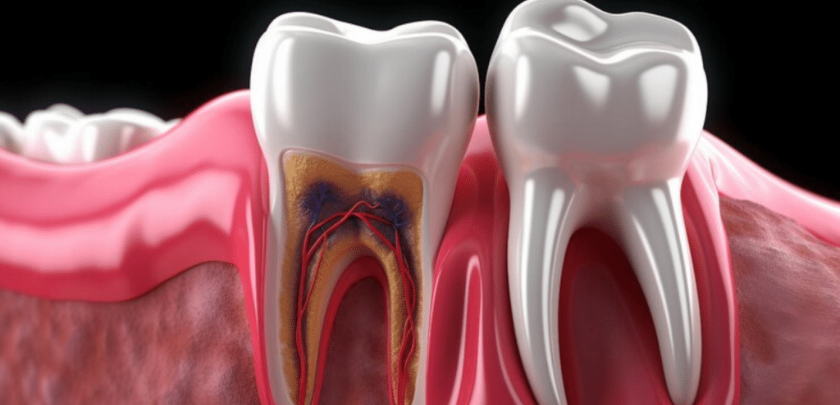
Most people are familiar with cavities that form on the chewing surfaces of teeth. Root cavities are a different and often more serious problem. They develop on the root surfaces of teeth, below where the enamel ends, and they tend to progress faster and cause more severe damage if left alone. Understanding what they are, what causes them, and how to catch them early can make a real difference in the treatment you ultimately need.
How Root Cavities Are Different from Regular Cavities
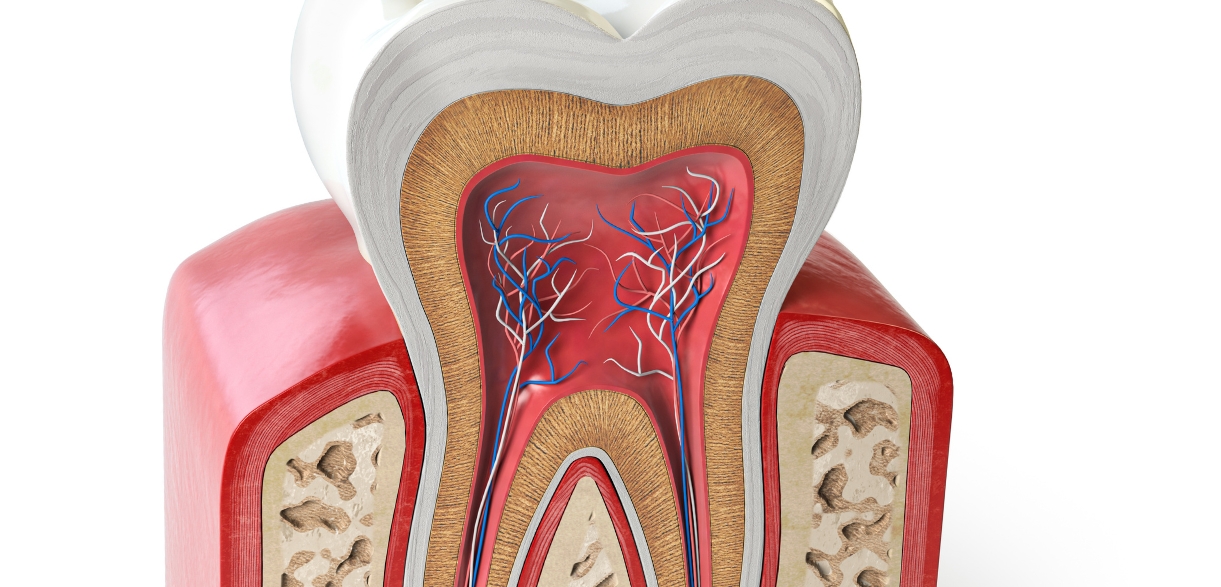
A cavity forms on the crown of the tooth – the visible portion protected by enamel, the hardest substance in the human body. Root cavities form on the exposed root surface, which is covered by a much softer material called cementum. Because cementum offers far less protection than enamel, decay on root surfaces advances more quickly and reaches the inner pulp of the tooth sooner.
This is why root cavities so frequently lead to more serious structural damage. Once decay reaches the pulp (the soft tissue at the center of the tooth containing nerves and blood vessels), root canal therapy becomes necessary to save the tooth from extraction. At Westinghouse Dental, patients dealing with advanced root decay regularly come in at this stage, often surprised at how quickly things progressed from a minor sensitivity to a full-blown dental emergency.
What Causes Root Cavities?
Root surfaces aren’t naturally exposed. When they become accessible to bacteria and acids, it’s almost always because something else went wrong first. Here are the main drivers:
Gum Recession
The gum tissue is designed to cover and protect the roots of your teeth. When it pulls back due to aggressive brushing, gum disease, or genetics, it leaves root surfaces open to the oral environment. According to the Journal of Periodontology, gum recession affects a large number of adults over 40. Once roots are exposed, they remain in contact with bacteria and acids in your mouth 24*7.
Periodontal Disease
Periodontal disease doesn’t just affect your gums – it destroys the bone and connective tissue that anchor your teeth. As the disease progresses, the root surfaces become increasingly exposed. The same bacterial environment driving your gum disease also accelerates root decay, which is why untreated periodontal disease and root cavities so often go hand in hand.
Dry Mouth
Saliva is your mouth’s natural defense system. It neutralizes acids, washes away food debris, and contains proteins that help protect tooth surfaces. Dry mouth caused by medication, systemic health conditions, or mouth breathing removes this protective layer. Without enough saliva, both roots and enamel become more vulnerable to acid attack. Hundreds of common medications list dry mouth as a side effect, making this a widespread and often overlooked risk factor.
Diet High in Fermentable Carbohydrates
Bacteria in your mouth feed on sugars and refined carbohydrates, producing acids as a byproduct. These acids lower the pH in your mouth and begin dissolving tooth structure, including root cementum. Frequent snacking, sugary drinks consumed throughout the day, and diets heavy in processed carbohydrates all contribute to an acidic oral environment that accelerates tooth decay.
Age
Root cavities are disproportionately common in older adults. This reflects a combination of factors: longer cumulative exposure to recession, a higher likelihood of taking multiple medications, and decades of dietary and hygiene habits adding up. The CDC notes that tooth decay remains prevalent across all age groups, but root cavities specifically trend sharply upward after age 50.
What causes cavities video source: TED-Ed YouTube Channel
Signs a Root Cavity May Be Developing
Root cavities don’t always announce themselves loudly, but there are warning signs worth paying attention to:
- Sensitivity to cold, heat, or sweet foods along the gumline is often the earliest signal. It may feel like a brief, sharp sting rather than a persistent ache.
- Tooth darkening or discoloration on the root surface near the gumline, often a tan, brown, or black spot, can indicate early decay.
- A rough or sticky feeling when running your tongue along the base of a tooth sometimes indicates surface breakdown.
- Toothache or prolonged sensitivity that doesn’t resolve on its own suggests the decay may have progressed closer to the pulp.
- Visible gum recession itself is a red flag, even before decay appears; exposed root surfaces are always at elevated risk.
Many of these early signs are subtle enough that patients miss them between dental visits, making consistent six-month checkups one of the strongest arguments. X-rays and clinical probing can detect root cavities in their early stages, when a filling or remineralization treatment may be enough.
Prevention: What Works
The good news is that root cavities are largely preventable with consistent, well-directed habits.
Protect Your Gum Line
If your gums are receding, address it. Switching to a soft-bristled toothbrush, correcting your brushing technique, and treating any underlying periodontal disease will slow or stop further recession. Less recession means less exposed root surface.
Use Fluoride
Fluoride helps remineralize both enamel and cementum, making them more resistant to acid. A fluoride toothpaste used twice daily forms the foundation of this. For patients at higher risk of gum recession, dry mouth, or a history of cavities, your dentist may also recommend a prescription-strength fluoride gel or varnish applied at regular intervals.
Stay Hydrated and Address Dry Mouth
Drinking plenty of water throughout the day supports healthy saliva flow. If a medication is causing dry mouth, ask your physician or dentist about whether alternatives exist or whether a saliva substitute might help. Chewing sugar-free gum with xylitol also stimulates saliva production and has some evidence supporting its role in reducing the risk of cavities.
Limit Acidic and Sugary Exposures
You don’t need to eliminate sugar entirely. Concentrated sugar exposure spread across the day (constant snacking, sipping sweet drinks) keeps oral pH low for longer stretches. Consolidating your sugar intake to mealtimes, rinsing with water afterward, and cutting back on between-meal snacks all meaningfully reduce root-surface acid exposure.
Keep Up with Professional Cleanings
No home routine fully replaces professional care. Cleanings remove tartar from root surfaces that brushing can’t reach, and your dentist can monitor early changes before they become cavities requiring intervention. Georgetown residents near the Westinghouse Dental office benefit from having local, consistent care they can return to regularly. Continuity matters when it comes to catching subtle changes year over year.
When Prevention Isn’t Enough
If a root cavity has already progressed into the pulp, root canal therapy is the standard treatment to save the tooth. The procedure removes the infected or damaged pulp tissue, cleans and seals the root canals, and is followed by a crown to restore the tooth’s function. It’s not the ordeal many people expect – modern techniques have made it far more comfortable than its reputation suggests.
Don’t wait for pain to tell you something is wrong. Book your appointment with Westinghouse Dental to find out where your oral health stands today.
People Also Ask
In the very earliest stage, when decay has only just begun softening the cementum surface without forming a true cavity, remineralization with fluoride treatments may halt or partially reverse the damage. However, once a cavity has formed (meaning there’s an actual hole or breakdown in the surface), it requires a filling. Your dentist can determine which stage you’re at with a clinical exam and X-rays.
Most patients report that the procedure itself is no more uncomfortable than getting a filling. The tooth and surrounding area are numbed thoroughly before treatment begins. Post-procedure soreness for a day or two is normal and manageable with over-the-counter pain relievers. The pain people associate with root canals usually comes from the infection that necessitated the procedure.
Root cavities progress faster than cavities on enamel surfaces because cementum is softer and thinner. In some cases, a root cavity can progress from early decay to pulp involvement within months, especially in a dry-mouth environment or with inconsistent oral hygiene. This is why early detection through regular checkups matters so much.
Yes, if you have gum recession that exposes root surfaces. Good hygiene significantly reduces your risk, but it doesn’t eliminate it if you have dry mouth, a diet high in acidic foods, or a structural recession that makes certain areas difficult to clean. Your dentist can identify your specific vulnerabilities and suggest targeted strategies.
Yes, and this is common. Root cavities in their early stages are frequently painless and invisible to the naked eye. They’re often discovered incidentally during routine X-rays or when a dentist probes the root surface during a checkup. By the time symptoms such as sensitivity, pain, and visible discoloration appear, the decay is usually already moderately advanced.